Austrian researchers have confirmed that a blood test can be used to monitor the healing of infections resulting from penetrating joint wounds.
A penetrating wound that breaches a joint’s synovial structure—the capsule that contains lubricating fluids—can be particularly devastating because the resulting inflammation and infection can lead to destruction of critical structures. The level of serum amyloid A (SAA) in the bloodstream has been successfully used to track inflammation in the body caused by other types of wounds and illnesses, so researchers at the University of Veterinary Medicine in Vienna set out to determine if it could provide similar information on penetrating joint injuries.
“SAA is an acute phase protein, which means that it is produced in the early phases of inflammation or infection and acts as an inflammatory mediator early in a disease process,” says Eva Haltmayer, Dr. Med. Vet.
Click here to learn what noisy joints may mean.
For the study, researchers followed the cases of 19 horses admitted to the university clinic for penetrating wounds to synovial structures that developed infection requiring surgical intervention to resolve. “The surgical treatment depended on the type of injury,” explains Haltmayer, “but basically the involved synovial structure was flushed, using either an arthroscope or with needles, and the wounds were also flushed and all dead tissue and debris were removed.” After surgery, horses were managed with antimicrobial and anti-inflammatory medications as needed and, if necessary, a second surgical procedure.
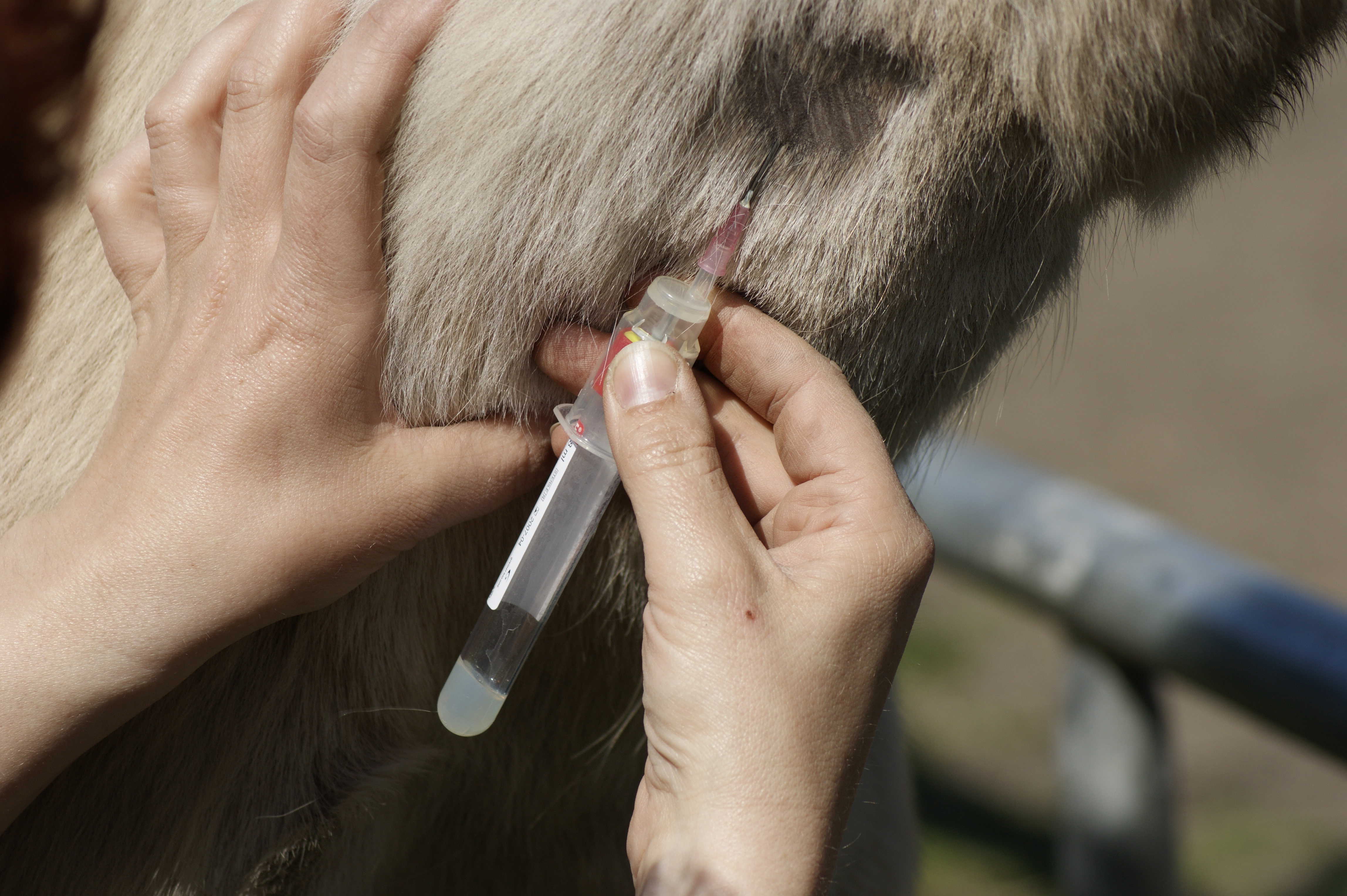
Blood samples were taken when the horses were admitted and again every 48 hours until the infection was considered resolved, and the SAA levels in each sample were documented. The researchers then compared changes in SAA levels to the course of the horse’s treatment and recovery.
The data showed that 12 study horses who required only one surgery showed a significant decrease in SAA levels after surgery and throughout the course of treatment. Specifically, they showed a 70 percent drop in SAA levels between hour 48 and hour 96 after surgery and a 99 percent drop by day six.
In contrast, the SAA levels varied much more over time among the four study horses who required a second surgery to clear infection. Two of the horses had high SAA levels that persisted after the initial surgery, and two had increased SAA levels after the first surgery. “Horses that needed a second surgery in our study still had an ongoing infection in the involved synovial structures,” says Haltmayer. “The presence of this infection was confirmed by analysis of the synovial fluid. It is not uncommon that horses with joint infection need several lavages of the involved synovial structure to resolve infection.”
The remaining three study horses had wounds that were less than 24 hours old prior to admission, so their SAA levels had not yet hit peak concentration prior to the start of the study, making any observed changes difficult to interpret. “Recently injured horses may initially show low values of SAA despite infection because not enough time has passed to reflect the full response,” says Haltmayer.
The researchers conclude that regular monitoring of SAA levels in plasma can be a useful tool in tracking effects of treatment of penetrating synovial injuries. However, says Haltmayer, whether the SAA tests can be used in diagnosis remains to be determined: “So far, we cannot recommend using SAA as a diagnostic marker for joint infection due to the very limited amount of patients in our study and the variety of in- juries. Further studies will be necessary to find out if SAA measured from peripheral blood can be used to specifically aid in detecting joint infection before signs are apparent.”
This article first appeared in EQUUS (Volume #480)
Don’t miss out! With the free weekly EQUUS newsletter, you’ll get the latest horse health information delivered right to your in basket! If you’re not already receiving the EQUUS newsletter, click here to sign up. It’s *free*!

